Today’s question revisits an earlier post – Paramedics and mandatory reporting (May 29, 2019) where my correspondent says that I:
… suggested that under the current reporting arrangements. a student paramedic who was found by paramedics suffering a drug overdose may be subject to a mandatory notification.
Given the new guidelines for treating practitioners announced for 2020, https://www.paramedicineboard.gov.au/Professional-standards/Mandatory-notifications.aspx, would the scenario play out the same way? My reading is that the paramedics would need to establish a direct risk to the public, or intoxication while practising to meet the burden for a mandatory notification. So, hypothetically, if the student was found suffering a drug overdose during their University break, while not on placement or even studying, can a credible risk to the public be established from a single interaction with paramedics. Likewise, would this same scenario apply to a student who sought treatment from their GP for an addiction-related issue.
How would you suggest people apply the test of establishing a “risk to the public”?
The Paramedicine Board has announced that
In 2020, the requirements to make a mandatory notification are changing. The changes aim to support health practitioners to be able to seek professional advice about their health without fearing a mandatory notification…
The changes apply to the mandatory notification requirements for treating practitioners – they do not affect the obligations of other registered practitioners (like colleagues), employers or education providers.
Under the changes, a treating practitioner only needs to make a mandatory notification about their practitioner-patient if there is a substantial risk of harm to the public from impairment, intoxication while practising, practice outside of accepted professional standards or where there is sexual misconduct.
This means that health practitioners who do not pose a substantial risk of harm to the public can seek professional advice without fear of a mandatory notification.
The new guidelines are not yet in place. A consultation paper was released on 11 September 2019 and the consultation period ended on 6 November 2019. As part of that process Draft revised Guidelines for mandatory notifications about registered health practitioners and Draft revised Guidelines for mandatory notifications about health students were released.
Although this question is about a student, it is the Draft revised Guidelines for mandatory notifications about registered health practitioners that is relevant. The ‘… notifications about health students’ guideline is about ‘students who, by undertaking a clinical placement with an impairment, are placing the public at substantial or very high risk of harm’. It specifically does not include reporting by treating practitioners (eg a paramedic who is called to assist a person who, by coincidence, is a paramedic student ‘suffering drug overdose during their University break, while not on placement or even studying’).
The ‘… notifications about registered health practitioners’ does deal with treating practitioners. It says (p. 11-14):
The conditions for treating practitioners to make mandatory notifications are more limited than they are for other people…
You must make a mandatory notification as a treating practitioner if, while treating another practitioner as your patient, you form a reasonable belief that they are:
- practising with an impairment
- practising while intoxicated by alcohol or drugs
- practising in a way that significantly departs from accepted professional standards, and
- engaging in sexual misconduct in connection with their practice…
With the exception of concerns about sexual misconduct, you should make a notification only if you believe there is a substantial risk of harm. A substantial risk of harm is a very high threshold for reporting risk of harm to the public. This allows practitioner-patients to seek and have treatment for conditions without fearing mandatory notification…
You may also need to make a mandatory notification about a student only if the student, doing clinical training with a serious and unmanaged impairment, is placing the public at substantial risk of harm…
If an impairment is related to or is a major cause of intoxication or departure from professional standards, consider how effective the practitioner-patient’s treatment is when you are deciding if it meets the very high threshold for reporting…
You must make a mandatory notification if you form a reasonable belief that your practitioner-patient is placing the public at substantial risk of harm (a very high threshold for reporting risk of harm) to the public by practising while intoxicated by drugs or alcohol.
The critical first question is ‘Do you have a reasonable belief that, by practising while under the influence of alcohol or other drugs the practitioner is detrimentally affecting their practice?’. The second question (see flowchart, p. 14) is ‘Do you have a reasonable belief that the intoxication is placing the public at risk of harm?’
Every situation is different but if a paramedic is called to a person who happens to be a paramedic student, and who is ‘suffering a drug overdose during their University break, while not on placement or even studying’ has to ask those questions and consider the factors in the guideline and shown below:
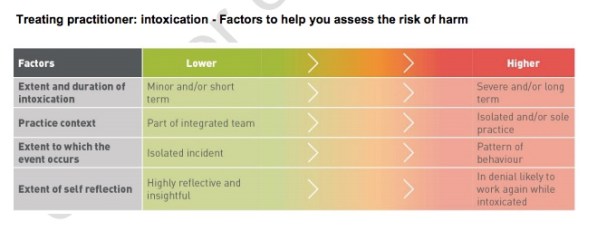
If you have no reason to think that the student has practised whilst intoxicated, if there is no reason to think that this anything other than an isolated short term incident rather than evidence of chronic persistent drug dependency then one might conclude there is no reason to believe that the person is or has practised whilst intoxicated or that their current intoxication is placing any patients at harm (given that, at the time, they are not practising). In that case as a treating practitioner you would not be required to report the person to AHPRA.
The same questions and risk assessment would indeed also apply to a GP who was treating a paramedic student for drug dependency. If the GP was satisfied that the student was ‘highly reflective and insightful’, was complying with prescribed treatment, was not intoxicated when at work, then he or she would not need to report the student to AHPRA. That conclusion would be consistent with the policy objective that ‘health practitioners who do not pose a substantial risk of harm to the public can seek professional advice without fear of a mandatory notification’.
I’m not sure if this conclusion is different to my earlier post. In that earlier post I said:
I shall assume, without debating it, that identifying the student paramedic has deliberately overdosed does give rise to a reasonable belief that the ‘student has an impairment that, in the course of the student undertaking clinical training, may place the public at substantial risk of harm’.
In my answer I did not address the question of whether a ‘a suspected [voluntary] drug overdose’ would or could give rise to the necessary belief that the ‘student has an impairment that, in the course of the student undertaking clinical training, may place the public at substantial risk of harm’. If the treating practitioner did not form the view that the patient’s intoxication gave rise to a belief that he or she was putting the public at risk, then there was no need to report the person to AHPRA. I did not address that question because I was addressing the question of whether a patient’s right to privacy was trumped by the mandatory reporting obligations where that belief did exist. In that earlier post I concluded that the obligation to report took precedence over the obligation to maintain patient confidentiality.
The draft guideline, when adopted, raises the bar to give greater weight to patient confidentiality and gives significant detail on how to assess that risk. It is still the case, however, that if the threshold belief of risk to the public is met, the obligation to report trumps the obligation to maintain confidentiality.
Conclusion
Remember that the draft guidelines are just that. When they are finalised and come into force, we are told sometime this year, people will need to familiarise themselves with the final version.
Assuming that the ‘in force’ guidelines will mirror the draft then a treating practitioner, GP or paramedic, will only need to report where he or she has a reasonable belief that,
- by practising while under the influence of alcohol or other drugs the practitioner is detrimentally affecting their practice; and
- that the intoxication is placing the public at risk of harm.
Can a credible risk to the public be established from a single interaction with paramedics? I would suppose that would depend on the history taken, what was said by the patient and others at the scene and the paramedic’s observations. It certainly could be possible if the student made admissions to practicing whilst intoxicated.
How would I suggest people apply the test of establishing a “risk to the public”? That question is answered, in detail, in the draft Guideline complete with examples. I would suggest people study that and refer to it should the need arise.
I have seen many patients in my time who are Healthcare Professionals with Mental Health illnesses who are genuinely forthcoming and have good insight and judgement into their illness to actively seek help and treatment for it. Almost all of them, as far as I am aware, are still actively practicing safely and professionally in their respective jobs, and are law-abiding and functional members of our society. I personally only facilitate a ‘Mandatory Report’ if there is a reasonably high risk that this person poses a risk to the public in their medical practice; or, there is an obvious self-admittence that they were intoxicated on the job or in an inappropriate relationship with a patient. I think Mandatory Reporting is a good thing to have such that it ensures no harm comes to patient safety and care from the people who are meant to be responsibly trating team, but at the same time, it shouldn’t be a barrier to allow Healthcare Professionals seek help for their own Mental Health issues which is evidently more prevelant in people who work in the medical field.